We covered three sessions today: a morning HRSA workshop on HIV care data, an afternoon session on the National HIV Curriculum (see below), and a lunchtime plenary session featuring speakers from federal agencies HRSA, CDC, NIH, and the HHS Office of HIV/AIDS and Infectious Disease Policy (see sidebar). The common theme: although remarkable improvements in HIV health outcomes have been made, our work is not over as disparities have been lessened but not eliminated.
Using Data to Improve Care
The quality of HIV care in the United States is improving steadily for myriad reasons. A key contributor to this success has been the extensive collection and use of data. The morning HRSA session, "Data Quality and Data Dashboards: Using Data to Improve HIV Care and Treatment," focused on the use of data for decision-making in HIV care—from the perspective of national-level efforts on the part of federal programs as well as the front-line work of three Ryan White HIV/AIDS Program (RWHAP) grant recipients.
The data under discussion are generated through a robust RWHAP client-level data system maintained by the HRSA HIV/AIDS Bureau (HAB). Insiders know this system as the RSR: the Ryan White Services Report, which generates detailed data reports on client characteristics and health outcomes in terms of measures such as levels of retention in care and degrees of success in viral suppression.
The session was moderated by Stacy Cohen, Chief of the HRSA Evaluation, Analysis, and Dissemination Branch. The branch is located within the HAB Division of Policy and Data.
Stacy Cohen, Dr. Carlos Salama, Dr. C. Ryan Tomlin, Pam Sylakowski
Using Data Nationally
RWHAP clients have better outcomes than individuals who do not receive care through RWHAP. Outcomes have improved across all population groups served by the RWHAP. However, disparities remain. Cohen highlighted some of the initiatives undertaken by HRSA to address these gaps, including technical assistance and training initiatives to improve care outcomes among black men who have sex with men, several projects to improve health through housing and employment, and projects to improve health outcomes along the HIV Care Continuum.
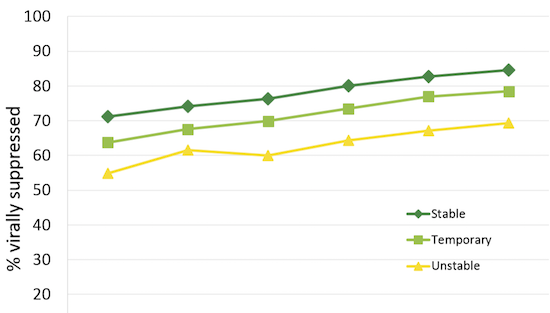
Improved Viral Suppression among RHAP Clients, by Housing Status, 2010‒2015
Data on the Front Lines
Elmhurst Hospital, New York City
Dr. Carlos Salama of Elmhurst Hospital Center in New York City said there is a "data disconnect" for grant recipients regarding the costs and time required to collect data in divergent formats generated through a variety of data software systems for different funders, which hampers the "ability to use this data to enhance care for our patients." One strategy to address these complexities is to generate monthly reports that provide physician-oriented data. Dr. Salama outlined a series of lessons learned (e.g., using reports to improve patient care) and data needs (e.g., standardized data reporting across funders). See the slides for more details.
Lessons Learned at Elmhurst
- Direct EHR data reports can have an immediate effect on patient retention by creating a systematic ability to track patients and ensure that they are making appointments, and to target specific patients to pursue for follow-up).
- A multidisciplinary team approach is needed to make use of these data.
Mercy Health, Grand Rapids, Michigan
Dr. C. Ryan Tomlin of Trinity Health in Grand Rapids, Michigan, reviewed features of his agency's data collection from various sources and its use in quality improvement, identification of disparities and formulation of responsive strategies, and ongoing patient monitoring. Tomlin highlighted the use of collected data for addressing various health needs. For example, to improve rates of HPV immunization, his agency takes data from a state registry and generates reports using CAREWare. Those reports are then used by nurses to order and schedule vaccination series at patients' subsequent clinic visits. However, that effort does not come without challenges, such as having reliable accessibility to the state database.
Tomlin also outlined use of data in tracking patient timeliness in securing prescription refills. "Follow-up calls are made by nurses and case managers to check-in or reengage patients in care." It works well, as the below chart shows in terms of improved viral suppression rates.
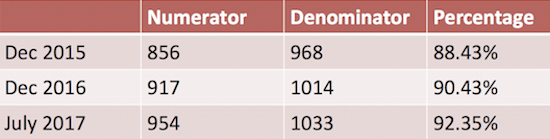
But challenges persist. For example, not all patients use his agency’s pharmacies, and there can be lags in refills due to unforeseen reasons such as hospitalization. Viral suppression rates have improved, and adherence strategies have been broadened in other clinic operations.
Nashville TGA, Tennessee
RWHAP Part A grant recipients are funders for hard-hit metropolitan areas. Pam Sylakowski, Director of the Nashville Transitional Grant Area (TGA), gave a system-wide perspective on use of data in decision-making. Successes cited by Sylakowski included direct access to the Enhanced HIV/AIDS Reporting System (eHARS), CDC's HIV/AIDS surveillance system.
Data can carry the message of people with HIV. Data can inspire action. Data can empower patients to manage their own health.
Nashville also has collaborated successfully with the Tennessee state Medicaid program on data sharing and developed a data monitoring tool to track accuracy of data quality in terms such as entry of client names and timeliness of data entry.
Sylakowski also cited several challenges, many of which have been addressed, at least in part. One was the need for simple reports that help make data "actionable" in decision-making, which has transpired through approaches like infographics (a HRSA infographic on RWHAP care outcomes was cited as a particularly useful tool) and one-page summary reports. Other challenges include the need to collect more client-level social indicator data, such as employment rates.
"We need data to design and deliver services. We can't wait until our data are perfect to act."
National HIV Curriculum
Dr. David Spach of the Mountain West AETC provided a review of HRSA's new National HIV Curriculum, a free educational website providing ongoing, up-to-date information needed to meet the core competency knowledge for HIV prevention, screening, diagnosis, and ongoing treatment and care to health care providers in the United States. The site was developed by the AIDS Education and Training Center Program National Coordinating Resource Center and the University of Washington and funded by HRSA. Free CME and CNE credits are offered throughout the site.
Dr. David Spach, Mountain West AETC and the University of Washington