Conference poster sessions are standard offerings at national meetings but, for some attendees, they get overlooked in the mix of workshops and plenaries and, well, eating and talking to colleagues. That’s why we are bringing a mini-recap of just a handful of the 154 poster sessions (not counting late breakers) from the 2016 Ryan White Conference. Our apologies if we missed you as there just wasn’t enough time to see everything.
St. Louis | Boston | Virginia | Portland | Oakland
St. Louis QI Reduces Missed Appointments
Washington University School of Medicine’s Part D Pediatric HIV clinic set up two quality improvement activities to realize great improvement in patient retention. Project One involved scheduling a future appointment before the client left the current appointment. While Project Two took active steps to schedule appointments for patients that were no shows or cancelled.
The results:
- Patients did better at keeping appointments. Those that did not keep a medical visit in the last 6 months dropped from 21% (2013) to 10% (2015)
- There was an uptick in retention when looking at a patients who kept medical visits throughout a 2 year period, from 71% (2013) to 76% (2015)
The Quality Improvement team attributes the changes to lessons learned like: fit within the existing workflow; bring in multiple staff and resources (including those outside the QI team); sharing responsibility for increasing appointment keeping; and more.
See the poster, Back to Basics: Using Quality Improvement Methodology to Impact Retention (Julia Schlueter, Maria Freshman, Ericka Hayes, Middy Estabrook, Phyllis Ballard, Kelly Nolan, Elizabeth Neuf, Washington University School of Medicine).

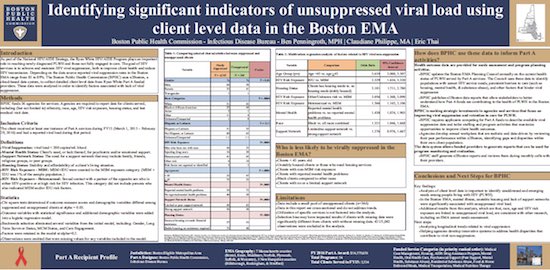
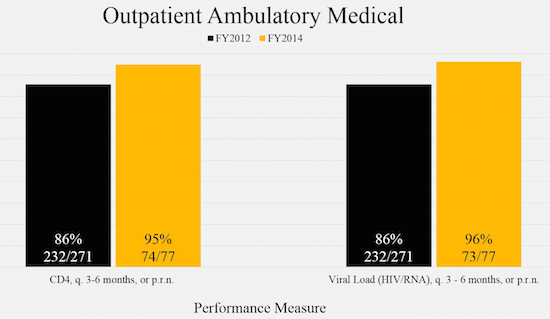
Boston Uses Client Level Data to Plan
Boston’s client-level data system, e2Boston, is used in identify barriers to viral suppression among individuals, a first step in population-based quality improvement.
The Boston Public Health Commission is the Part A grant recipient and oversees 36 Ryan White Part A-funded agencies in the metro area. e2Boston data are used, for example, for Planning Council review and decision-making and analyzed by agencies to help them develop annual work plans to develop quality improvement plans to increase rates of viral suppression.
See the poster: Identifying Significant Indicators of Unsuppressed Viral Load Using Client Level Data in the Boston EMA (Ben Penningroth, Claudiane Philippe, Eric Thai, Boston Public Health Commission).
Virginia Review Teams Enhance Quality of Care
Virginia's Part B RWHAP program created a Peer Review team to conduct a quality improvement process that examined HIV care delivery by agencies funded by the Virginia RWHAP Part B state program. The team was comprised of experts from across the state, who reviewed data from agencies, using service standards and review modules to guide the process. The team went to site visits to 15 agencies (2015-2016) and, after each visit, convened a collaborative meeting to identify strengths and weaknesses. Significant improvements were identified in terms of the HIV care continuum (improved viral load and CD4 testing), oral health assessments and referrals as well as increases in case management contacts and services.
See the poster: Quality Management Through a Collaborative Learning Process: Virginia Ryan White Part B Peer Review (Michelle Shearer, D’Juan Waller, Suzanne Lavoie, Safere Diawara, Virginia Commonwealth University and Virginia Department of Health)
Portland Visualizes Paths to Viral Suppression
This poster presents a "line-of-site diagram for various service categories and how they work towards achieving viral suppression. The graphic was prepared by the Portland-Multnomah County Oregon Part A Transitional Grant Area.
See the poster, Line of Sight Towards Viral Suppression (Amanda Hurley, Marisa McLaughlin). See also the related workshop: Fostering the Clinical Quality Management Program Using Quality Improvement Practices.

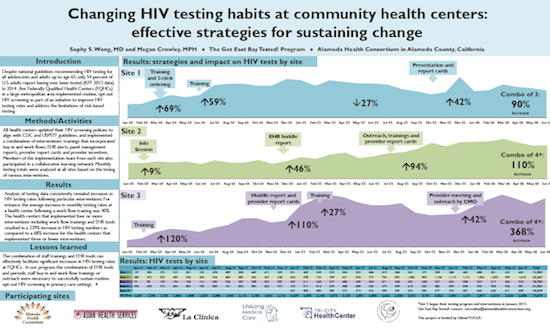
Oakland Increases HIV Testing at Health Center Sites
Five HRSA-funded Federally Qualified Health Centers (FQHCs) in the Oakland area implemented federally-recommended routine opt-out HIV screening to broaden HIV testing among their patient populations. All five FQHCs updated their HIV screening policies to reflect federal guidelines and participated in a collaborative learning network.
A combination of the following interventions were adopted:
- Trainings to promote buy-in and work flow adjustments
- Electronic Health Record (EHR) alerts
- Panel management reports
- Provider report cards
- Provider incentives
Unsurprisingly, those adopting more interventions saw larger increases in HIV testing, with trainings and EHR tools being particularly valuable.
See the poster: Changing HIV Testing Habits at Community Health Centers: Effective Strategies for Sustaining Change (Sophy Wong, MD, Megan Crowley, Alameda Health Consortium).